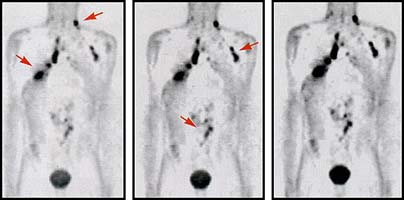
 In this image the PET scan shows a chain of lymph node tumors in the neck, chest an abdomen. The tumors are visible because the patient was injected with a glucose tracer which collects in the highly metabolic cancer cells. All cells use glucose to thrive but cancer cells, because they are rapidly growing cells, are glucose hogs. This is why the cancer cells are easily seen on the PET scan. Results of PET Scan May Alter Cancer Treatment, By Merritt McKinney NEW YORK (Reuters Health) - A scan that looks for cancerous activity throughout the body may help doctors decide on the best treatment for cancer patients, researchers in Hawaii report. In two surveys, a whole-body scan called FDG-PET, or fluorodeoxyglucose positron emission tomography, was useful in making treatment decisions in 89% to 96% of patients. Besides helping doctors decide whether a suspicious mass or lump is cancerous, "for those people who are already being treated for cancer, PET can change the course of care in most cases," the study's lead author, Dr. Robert Tucker of Queen's Medical Center in Honolulu, told Health. With the aid of a PET scan, doctors can choose the most appropriate drugs and procedures, which may improve patients' quality of life, he explained. FDG-PET scans work by measuring the use of glucose, or sugar, in the body's cells. Since cancer cells consume more sugar than normal cells, the scan identifies cancerous cells in the body and shows whether cancerous cells have spread beyond the original location of a tumor. In a group of 463 cancer patients who underwent FDG-PET, the scan was valuable in making or confirming treatment decisions in 89% of patients, Tucker and his colleagues report in the May 1st issue of the Journal of Clinical Oncology. And in 45% of the patients, doctors changed the recommended treatment based on what the scan showed. The most common type of cancer in the survey was lung cancer, followed by head and neck cancer, and colorectal cancer. In a sample of 53 mostly lung-cancer cases pulled from the larger group to be reviewed by a lung specialist and a cancer surgeon, FDG-PET scans were even more helpful, according to the report. The screens were judged useful in 96% of the cases. In 33% of patients, surgery was canceled after doctors reviewed the results of the scan. In 15% of patients, chemotherapy or radiation was added to the treatment plan afterwards, and one or more of the treatments was canceled in 7% of patients. Based on the results of the surveys, Tucker said that FDG-PET "should become an integral part of a physician's diagnostic work-up of a suspected cancer patient and a routine exam for those with cancer." Although FDG-PET scans are expensive to perform, Tucker and his colleagues suspect that the test is worth the extra cost, since it can rule out unnecessary treatment. Tucker's group is now conducting a 2-year study comparing the treatment costs of patients who have PET scans with other patients who do not undergo the tests. SOURCE: Journal of Clinical Oncology 2001;19:2504-2508. |